TYPES OF ACL RECONSTRUCTION GRAFTS
There are many variations of ACL reconstruction, all of which aim to give the patient the best functioning knee possible. The variability depends on what the graft, the new ligament, is made from. In general, there are three main graft options: a patellar tendon autograft, a hamstring autograft, and an allograft. An autograft comes from the patient’s own body, whereas an allograft comes from a cadaver donor. An allograft can come from patellar tendon, hamstring tendon, achilles and other ankle tendons. When deciding which graft to use for a patient’s reconstruction, age, lifestyle, preference, and the surgeon’s familiarity with certain grafts should all be discussed. While extensive studies have been completed comparing the effectiveness of different grafts in patients, it is important to remember that the best graft for one person may not be the right choice for you, and your individual needs should be discussed with your doctor.
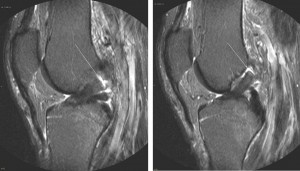
Patellar Tendon Autograft
A patellar tendon autograft involves harvesting the central one-third of the patellar tendon from your injured knee. The patellar tendon connects the patella, or kneecap, to the tibia, or shinbone. When the graft is harvested a small piece of bone is taken from the patella and the tibia, making it a bone-tendon-bone graft. The graft is inserted into the knee to form a new ACL using screws, and eventually the graft bone fuses with the surrounding bone of the femur and tibia. An advantage of the patellar tendon graft includes a strong initial fixation. Additionally, studies have shown that the patellar tendon eventually regenerates in the donor knee. Harvesting the patellar tendon does increase the risk for patellar tendon rupture or patellar fracture in the donor knee in the initial months after surgery, and the risk of developing patellofemoral pain, and stiffness, which could require additional physical therapy in the future.
Hamstring Autograft
The hamstrings are a group of tendons that connect to the hamstring muscles of the back of the thigh. When a hamstring autograft is used, two of these tendons are removed and bundled together using sutures to create a tissue graft. The hamstrings are generally taken from the leg undergoing ACL reconstruction. Advantages of this method include a very small incision to harvest the tendon, and less risk of developing patellofemoral pain or patellar tendon rupture. Though the hamstring graft does not have as strong of a fixation as the bone-to-bone fixation of the patellar tendon graft, the fixation is still very strong, and fixation methods are being improved upon all the time. Additionally, like the patellar tendon, hamstring tendons also regenerate.
Allograft
An allograft taken from a cadaver donor is also commonly used for ACL reconstruction. Though studies have shown an allograft is not quite as strong as a patient’s own tissue, for a non-competitive athlete an allograft can function at a very high level, and allow a patient to return to their desired sports and activities. Advantages of allografts include a decreased operative time, less post-operative pain, and no need for harvesting incisions. Because the tissue comes from someone else, there is always a miniscule risk of contracting a disease from the tissue. However, advancements in screening and sterilization make this risk exceedingly small. Additionally, because these grafts are thoroughly washed and contain very little protein antigen, the risk of graft rejection is also very small. Allografts are well suited for casual athletes, athletes over 40, revision or repeat ACL surgery and those who absolutely prefer minimally invasive surgery.
Schedule a Consultation with Dr. Millstein
Dr Millstein has extensive experience with all types of grafts for ACL reconstruction and revision ACL reconstruction. He feels it is very important to individualize treatment and is always willing to discuss your preferences. If you are considering an ACL surgery and want to discuss which graft option would most benefit you, call (310) 595-1030 and schedule a consultation with an expert orthopedic and sports medicine surgeon.

